Summary
- Working as an OFW caregiver is emotionally and physically demanding, especially when dealing with aggressive or uncooperative patients.
- Caregivers are in high global demand, with strong salary and migration opportunities in countries like Canada and Australia.
- Learning de-escalation techniques, communication skills, and self-protection strategies is essential to stay safe and keep your job.
- Education, language training, and proper credential recognition are key to accessing higher-paying caregiver roles abroad.
- With the right mindset and preparation, Filipino caregivers can turn difficult patient encounters into a sustainable, respected global career.
Introduction
For many Filipinos, becoming an OFW caregiver is the ultimate sacrifice to provide a better future for their families. It is a calling that combines hard work, compassion, and the hope of long-term migration opportunities.
However, the “heart of a caregiver” is often tested by patients who are uncooperative, aggressive, or demanding. These situations can be shocking for first-time OFWs who only imagined smiling elderly clients and grateful families.
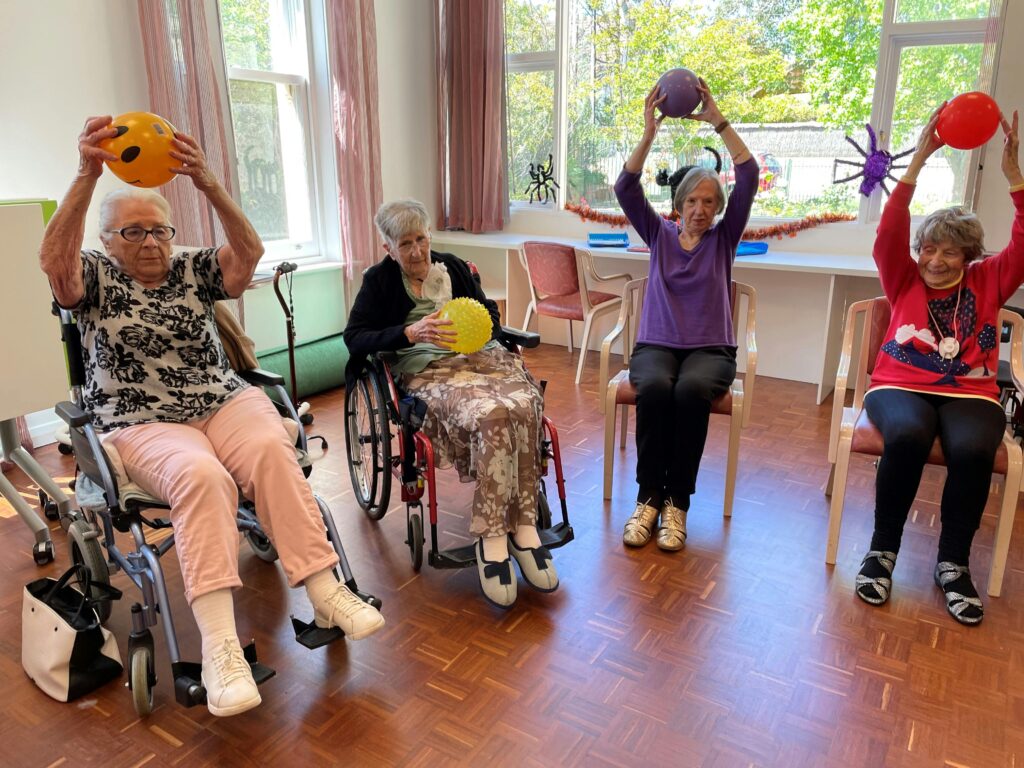
This article provides a professional roadmap on how to manage these challenging interactions without losing your composure or your job. We combine practical de-escalation techniques with a realistic look at the caregiver industry in 2026 so you are prepared for the world stage.
Job role overview
As a caregiver (often called a Personal Care Worker, Support Worker, Aged Care Worker or Home Health Aide), you are the primary support system for individuals who cannot fully care for themselves due to age, illness, or disability.
Core responsibilities:
- Assisting with Activities of Daily Living (ADLs) such as bathing, dressing, feeding, and toileting
- Providing mobility support, including transfers from bed to chair and walking assistance
- Giving medication reminders (not prescribing, but ensuring correct timing and dosage as instructed)
- Offering emotional companionship and social interaction
- Observing and reporting changes in the patient’s condition to nurses or supervisors
Typical work environments:
- Private homes (home care or live-in arrangements)
- Aged care facilities and nursing homes
- Assisted living centers and group homes
Equipment used:
- Patient hoists and lifts for safe transfers
- Wheelchairs, walkers, and mobility aids
- Blood pressure monitors, thermometers, and pulse oximeters
- Digital charting apps and tablets for real-time reporting and documentation
Salary comparison abroad (2026 projections)
Caregiving is a high-demand, stable career with pay scales that vary based on cost of living, local labour laws, and whether you work in public or private facilities.
| Country | Average Annual Salary | PHP Equivalent (Approx.) | Entry-Level Pay |
|---|---|---|---|
| Australia | $55,000 – $72,000 AUD | ₱2.1M – ₱2.7M | $28 – $32 per hour |
| Canada | $40,000 – $58,000 CAD | ₱1.7M – ₱2.4M | $18 – $23 per hour |
| United Kingdom | £24,000 – £32,000 GBP | ₱1.7M – ₱2.3M | £11 – £14 per hour |
| Japan | ¥2.4M – ¥3.6M JPY | ₱900,000 – ₱1.4M | ~¥1,000 per hour |
| UAE / Saudi Arabia | $7,200 – $15,000 USD | ₱400,000 – ₱850,000 | Tax-free monthly salary |
Overtime: In Western countries, overtime is abundant and often paid at 1.5x the base rate, especially for night shifts, weekends, and holidays.
Tax considerations: Income tax is higher in Australia and the UK (around 15–30%), while income in the Middle East is usually tax-free but with fewer PR options.
Demand and job outlook
Top hiring countries in 2026:
- Canada: New caregiver PR pathways and pilot programs.
- Australia: Severe aged care worker shortage, especially in regional areas.
- Germany: Language-subsidised programs for foreign care workers.
- Japan: Ongoing need through TITP and care-specific programs.
Career stability: Very high. The “Silver Tsunami” (aging global population) ensures that caregivers will be needed for decades.
AI risks: Low. Robots may assist with lifting or reminders, but empathy, cultural sensitivity, and human presence cannot be replaced by AI.
Education and certification requirements
Philippine standard: TESDA Caregiving NC II is the minimum requirement for DMW processing for most caregiver roles.
Credential recognition abroad:
- Canada: Often requires an Educational Credential Assessment (ECA) and English at CLB 4–5 or higher.
- Australia: Certificate III in Individual Support (Ageing or Disability) is commonly required; some employers sponsor this training.
- Japan: Requires language training (usually N4–N3 level) and specific care training under their programs.
Language requirements:
- IELTS General (band 4.5–5.5) or equivalent PTE score for many Western visas.
- Local language basics (German, Japanese, etc.) for non-English-speaking countries.
Cost and time to qualify
Study duration: Around 6 months for TESDA Caregiving NC II, plus 2–3 months for language review and visa preparation.
Tuition costs in the Philippines:
- ₱15,000 – ₱35,000 depending on school, location, and inclusions (OJT, uniforms, materials).
Visa and processing costs:
- ₱150,000 – ₱300,000 including medical exams, documentation, language tests, and airfare.
- Many 2026 programs, especially in Canada and Australia, are partly or fully employer-paid, reducing upfront costs.
Career growth opportunities
Advancement options:
- HCA-to-LPN (Licensed Practical Nurse) bridging programs in Canada and the US.
- Progression to senior or “Lead Support Worker” roles in facilities.
- Transition into care coordination, team leader, or supervisor roles.
Specialisations:
- Dementia and Alzheimer’s care
- Palliative and end-of-life care
- Disability support and behavioural care
Salary progression: Moving from a general caregiver to a lead or specialised support worker can increase pay by 20% or more, especially in structured systems like the UK and Australia.
Work-life balance and job stress
Physical demands: High. There is a real risk of back injuries and joint problems from frequent lifting, transfers, and long hours on your feet.
Shift schedules:
- Rotating shifts (morning, afternoon, night) are common.
- 12-hour shifts are standard in many UK and Canadian facilities.
- Live-in home care roles may blur the line between work and rest time.
Burnout levels: Very high. Constant exposure to illness, death, and difficult behaviours can lead to “compassion fatigue” if self-care is ignored.
How to handle difficult and aggressive patients
Difficult patients are not a sign that you are a bad caregiver. They are a normal part of the job, especially in dementia, mental health, or chronic pain settings. The key is to respond professionally, not emotionally.
1. Understand the root cause
- Dementia or confusion: Patients may hit, shout, or resist care because they are scared or disoriented.
- Pain: Chronic pain can make anyone irritable or aggressive.
- Loss of independence: Many elderly patients feel embarrassed needing help with bathing or toileting.
When you see behaviour as a symptom, not a personal attack, it becomes easier to stay calm.
2. Use calm, simple communication
- Speak in a low, steady voice.
- Use short, clear sentences: “Mr. John, I am here to help you stand up safely.”
- Avoid arguing or raising your voice, even if the patient is shouting.
3. Maintain safe body positioning
- Stand slightly to the side, not directly in front of an agitated patient.
- Keep an arm’s length distance if they are likely to hit or grab.
- Know where the exit is in case you need to step away quickly.
4. Use distraction and redirection
- Change the topic to something they like (family, hobbies, favourite food).
- Offer a drink of water or a small snack if allowed.
- Suggest a different activity and return to the task later when they are calmer.
5. Set gentle but clear boundaries
- Use phrases like: “I want to help you, but I cannot if you hit me.”
- Reassure them: “You are safe. I am here to support you.”
6. Always report and document incidents
- Inform your nurse or supervisor immediately if a patient hits, kicks, or threatens you.
- Write an incident report as required by facility policy.
- Never hide injuries or serious incidents; documentation protects both you and the patient.
7. Protect your mental health
- Talk to trusted co-workers about difficult shifts.
- Use your days off to truly rest, not just send money and worry.
- Consider journaling or online support groups for caregivers.
Pros and cons (side-by-side)
| Pros | Cons |
|---|---|
| Fastest pathway to permanent residency in countries like Canada and Australia. | High physical and emotional toll from constant patient care. |
| Stable income with strong overtime potential. | Risk of verbal or physical aggression from patients. |
| High respect for Filipino caregivers and their compassion. | Living in employer’s home (for stay-in roles) can feel isolating. |
Which path is better for you?
Scenario A – Fastest deployment: Aim for the Middle East or Japan (TITP or care programs). Processing is quick, but permanent residency is less likely.
Scenario B – Highest long-term salary: Pursue Australia. The 2026 wage hikes for aged care workers make it one of the most lucrative destinations.
Scenario C – Family reunification: Canada remains the best option for bringing your spouse and children earlier, especially under caregiver PR pathways.
Common mistakes Filipino applicants make
- Taking it personally: Forgetting that aggression in elderly patients is often a symptom of dementia, confusion, or pain.
- Ignoring ergonomics: Not using patient lifts or proper techniques because they are “in a hurry,” leading to lifelong back pain.
- Underestimating language barriers: Struggling with local accents (Australian, Scottish, etc.) and slang, which affects their ability to calm patients.
- Skipping self-care: Working nonstop overtime and burning out within a year.
Frequently asked questions (FAQ)
Can I work as a caregiver if I am a Nurse in the Philippines?
Yes. Many Filipino nurses start as caregivers or support workers abroad as a stepping stone to faster deployment and later transition to nursing roles.
What do I do if a patient hits me?
Immediately step back, ensure your safety, inform your supervisor, and document the incident. Most countries have clear policies protecting workers from workplace violence.
Is there a height or weight requirement?
Not officially, but you must pass a physical “Fit to Work” exam and be able to perform safe patient handling tasks.
Do I need a college degree?
Not always. For Canada, a one-year post-secondary credential or equivalent is usually required, but some programs accept TESDA NC II plus experience.
What is the best way to calm an angry patient?
Use a low, calm voice, maintain respectful eye contact, avoid arguing, and try to understand what is triggering their frustration.
Can I bring my family?
In countries like Canada and the UK, it is possible depending on your visa type, salary level, and program rules.
Conclusion
Handling difficult patients is an inevitable part of being a professional caregiver, especially on the global stage. The key is not to avoid these situations, but to be prepared for them—physically, emotionally, and professionally.
By mastering de-escalation techniques, protecting your own safety, and choosing a country that aligns with your long-term goals, you can turn a challenging job into a rewarding international career. Your compassion is your strength, but your boundaries and skills are your protection.
Remember: your safety is as important as the patient’s care. A prepared Filipino caregiver is not just a worker abroad, but a respected professional anywhere in the world.
FAQ: How Filipino Nurses Can Handle Difficult Patients
1. Why do some patients become difficult or aggressive?
Patients may act out due to pain, fear, anxiety, medication effects, confusion, or frustration with their condition. Their behavior is often a reaction to stress rather than a personal attack on the nurse.
2. How should nurses respond to rude or angry patients?
Stay calm, maintain a professional tone, acknowledge their feelings, and set clear boundaries. Avoid arguing and focus on understanding the root cause of their frustration.
3. What communication techniques help with difficult patients?
Use active listening, empathy statements, simple explanations, and a calm voice. Techniques like the “LEAP” method (Listen, Empathize, Apologize, Problem-solve) are effective in de-escalating tension.
4. How can nurses protect themselves during aggressive situations?
Maintain a safe distance, position yourself near an exit, call for assistance, and follow hospital protocols for violent or unpredictable patients. Safety should always come first.
5. How do Filipino nurses stay emotionally strong when dealing with difficult patients?
By practicing self-awareness, taking short breaks when possible, seeking support from colleagues, and reminding themselves that patient behavior is often driven by illness, not intention.
6. What should nurses avoid when handling difficult patients?
Avoid raising your voice, taking comments personally, making threats, or showing frustration. These reactions can escalate the situation and damage trust.
7. How can nurses build rapport with challenging patients?
Show consistency, respect, and patience. Small gestures like explaining procedures clearly, checking in regularly, and using the patient’s name help build trust over time.
8. When should nurses escalate the situation to supervisors or security?
Escalate when a patient becomes physically aggressive, threatens harm, refuses to calm down, or when the situation feels unsafe. Hospitals have protocols to protect both staff and patients.